The name may sound pleasing but it’s really not — sweet syndrome is actually a rare disease that causes red lumps to appear on the skin. Named after Dr. Robert Douglas Sweet who first described it way back in 1964, it’s not contagious and there are treatments available for it.
Experts say that treatments for sweet syndrome tend to cause rapid improvements in the symptoms. And when the red lumps go away, they really go away — they do not leave behind scars. However, there are some cases wherein the disease is highly resistant to treatments.
Also known as acute febrile neutrophilic dermatosis, it commonly affects middle-aged females. Men and the elderly may also suffer from the skin disease, too. It may also occur in children, although it rarely happens.
No one really knows what causes sweet syndrome, but doctors suspect that it is more common in people with a particular genetic marker, which is HLA B54. It is possible for the appearance of the disease to follow certain occasions or medical conditions — some of them will be discussed later on in this article.
Signs and Symptoms
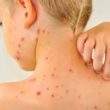
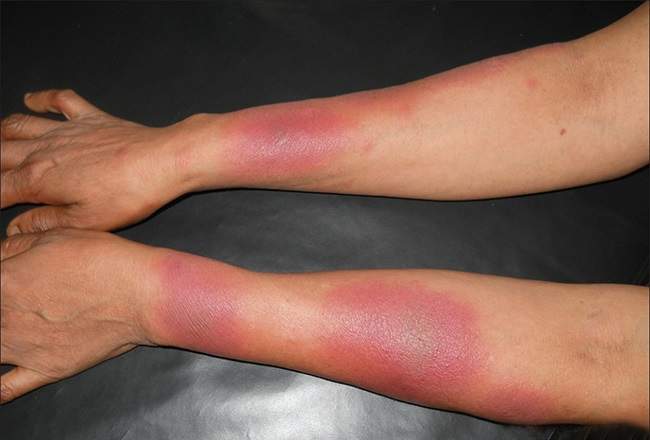
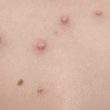
One of the telltale signs of sweet syndrome is the presence of red lesions that form on the skin. They can vary in appearance, sometimes appearing as flat patches and other times looking more like blisters. Only a few lesions may form, but it’s possible for them to be numerous.
Tender and painful, these lesions usually appear on the neck and limbs although other areas of the body may be affected as well. Also, lesions may form on mucous membranes such as the inside of the mouth or on the tongue.
Aside from skin and mucosal lesions, there are a few more signs and symptoms associated with sweet syndrome. Some of them include malaise (a general feeling of being ill), tiredness, and moderate to high fever. It’s not unlikely for a person with sweet syndrome to have headaches, achy joints and sore eyes.
Causes and Risk Factor
To date, no one can tell the exact reason behind sweet syndrome. However, experts say that individuals with the genetic marker HLA B54 are more commonly bugged by the skin disease. They add that pro-inflammatory cytokines (substances secreted by the cells of the immune system that fire up systemic inflammation) are role players, too.
Sweet syndrome is commonly seen in middle-aged women, but older females can have it as well. Men and children, although very rarely, may also suffer from the disease. It’s possible for sweet syndrome to affect a previously healthy person, although it can be attributed to the presence of an underlying medical condition or systemic infection.
It’s not unlikely for sweet syndrome to be triggered by things such as excessive sun exposure, pregnancy and even getting vaccinated. There are many health problems that may cause the disease to arise. Some of them include upper respiratory tract infections, rheumatoid arthritis, blood disorders, inflammatory bowel diseases, and GI tract infection. Sometimes, a weakened immune system and the intake of certain medications may be blamed as well.
Medical Treatment
The use of systemic corticosteroids is one of the most preferred treatments for sweet syndrome. Within a few days of the drug’s administration, the skin lesions as well as fever go away. In other words, systemic corticosteroids can cause a rapid improvement of the signs and symptoms sweet treatment brings.
It’s not all the time, however, that systemic corticosteroids are effective. If such is the case, a doctor may choose to treat the skin disease with the use of other medications. Some of them include topical or intralesional corticosteroids, potassium iodide solution and indomethacin, which is a non-steroidal anti-inflammatory drug (NSAID).
Most of the time, the occurrence of sweet syndrome happens only once. However, 1/3 of people who suffer from it may encounter recurring episodes, in particular patients with certain medical conditions such as cancer.